HOW TO LIVE WITH PSORIATIC ARTHRITIS
What is Psoriatic Arthritis?
Psoriatic arthritis is a type of arthritis linked with psoriasis, a chronic skin and nail disease. Psoriasis causes red, scaly rashes and thick, pitted fingernails. Psoriatic arthritis is similar to rheumatoid arthritis (RA) in symptoms and joint swelling (inflammation). But it tends to affect fewer joints than RA. And it does not make the typical RA antibodies. The arthritis of psoriatic arthritis comes in 5 forms:
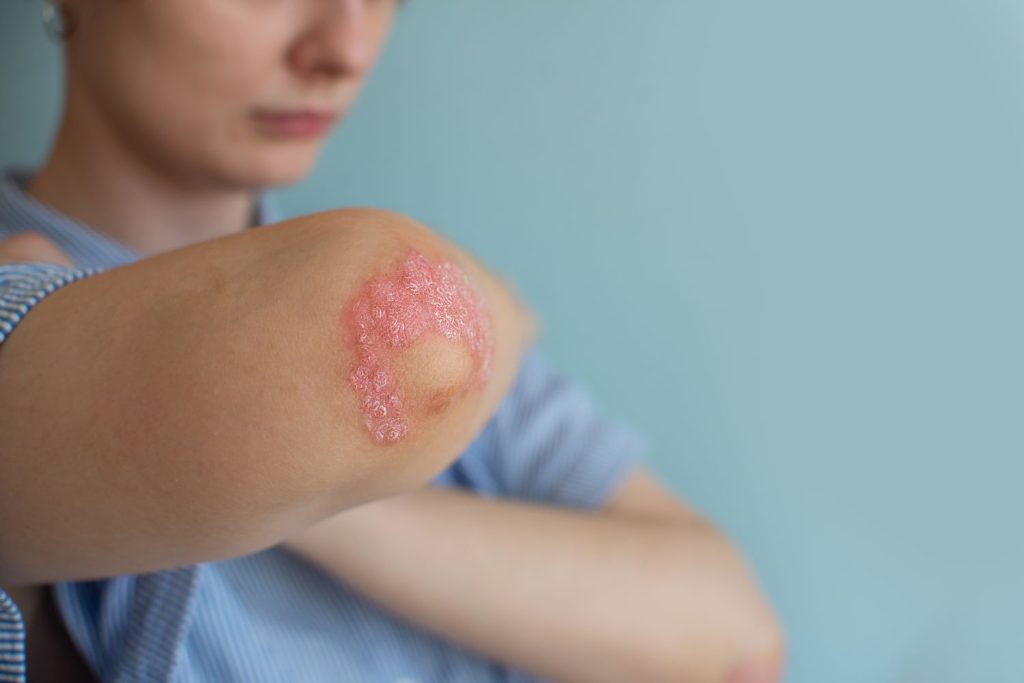
- Arthritis that affects the small joints in the fingers, toes, or both
- Asymmetrical arthritis of the joints in the hands and feet
- Symmetrical polyarthritis, which is similar to RA
- Arthritis mutilans, a rare type of arthritis that destroys and deforms joints
- Psoriatic spondylitis, arthritis of the lower back (sacroiliac sac) and the spine
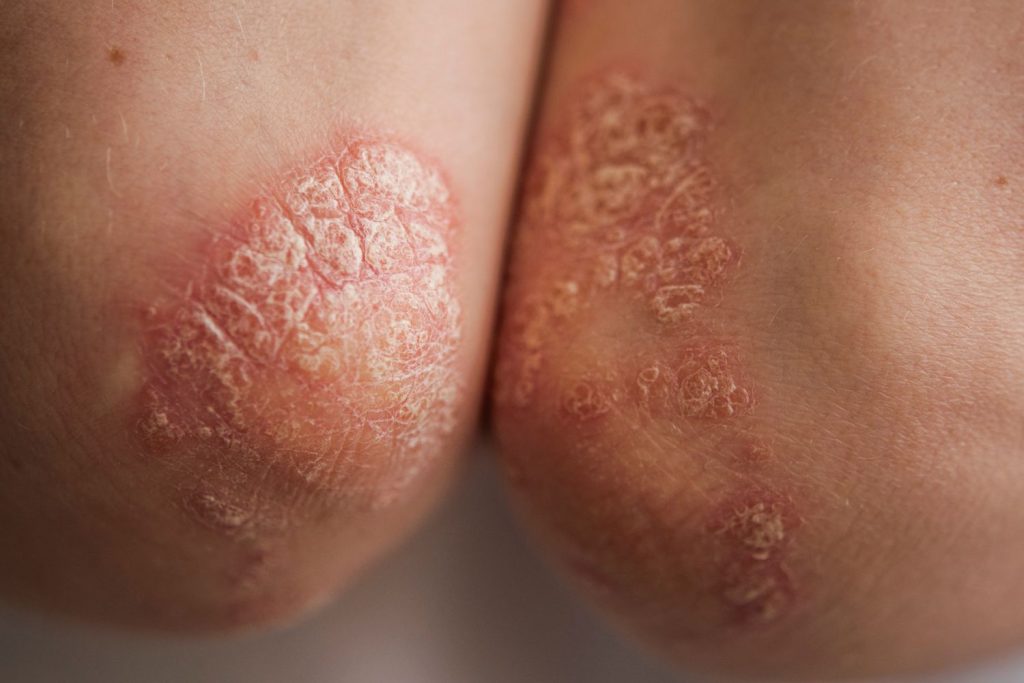
What causes Psoriatic Arthritis?
Doctors don’t know what causes psoriatic arthritis. But factors such as immunity, genes, and the environment may play a role.
What are the symptoms of Psoriatic Arthritis?
The psoriasis symptoms may start before or after the arthritis. Psoriasis causes red, scaly rashes and thick, pitted fingernails. About 3 in 20 to 3 in 10 people with psoriasis may develop psoriatic arthritis. Symptoms of psoriatic arthritis may include:
- Inflamed, swollen, and painful joints, often in the fingers and toes
- Deformed joints from chronic inflammation
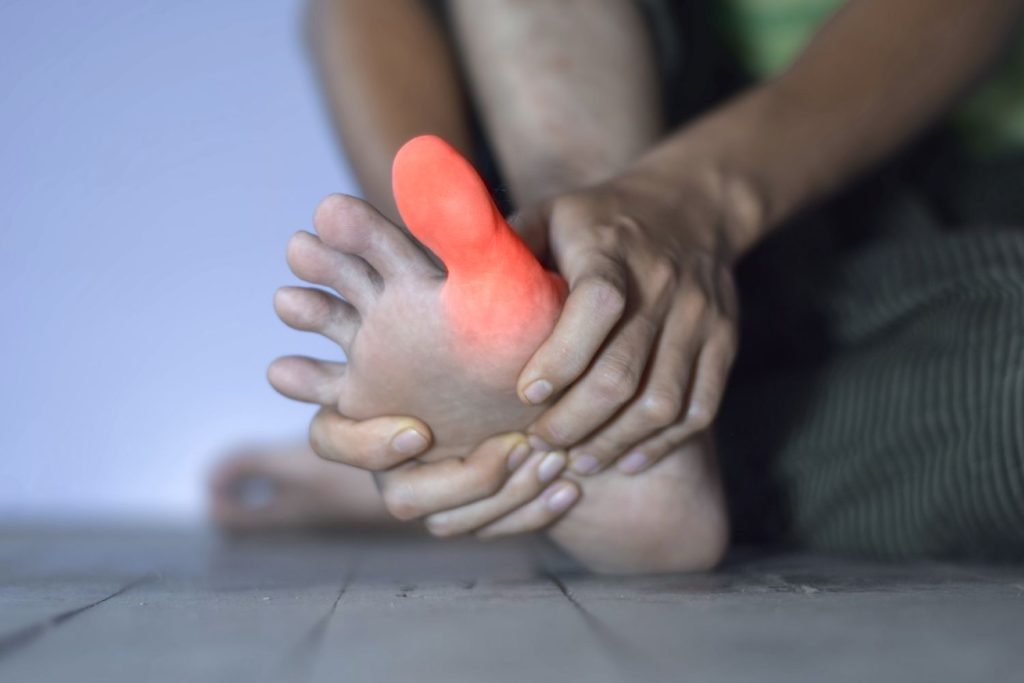
The symptoms of psoriatic arthritis can look like other health conditions. Make sure to see your healthcare provider for a diagnosis.
Diagnosis
Psoriatic arthritis is easier to confirm if you already have psoriasis. If you don’t have the skin symptoms, diagnosis is more difficult. The process starts with a health history and a physical exam. Your healthcare provider will ask about your symptoms. You may have blood tests to check the following:

- Erythrocyte sedimentation rate (ESR or sed rate). This test looks at how quickly red blood cells fall to the bottom of a test tube. When swelling and inflammation are present, the blood’s proteins clump together and become heavier than normal. They fall and settle faster at the bottom of the test tube. The faster the blood cells fall, the more severe the inflammation.
- Uric acid. High blood uric acid levels can be seen in psoriatic arthritis but are not used for diagnosis or monitoring.
- Imaging. X-rays, CT scans, ultrasound, MRI, and skin biopsies may all be used to help diagnosis.

How is Psoriatic Arthritis Treated?
Treatment will depend on your symptoms, age, and general health. It will also depend on the severity of your condition.
Both the skin condition and the joint inflammation are treated. Early diagnosis and treatment helps prevent joint damage. Some medicines used to treat psoriatic arthritis include:
- Nonsteroidal anti-inflammatory medicines (NSAIDs) to ease symptoms
- Corticosteroids for inflammation
- Immunosuppressive medicines such as methotrexate to reduce inflammation if NSAIDs don’t work
- Biologic medicines to ease inflammation
- Vitamins and minerals such as calcium and vitamin D to slow bone deformation
Other treatment may include:
- Exercise
- Heat and cold
- Occupational therapy to help you do your daily activities
- Physical therapy to help your muscle and joint function
- Management of psoriasis skin rash
- Splints
- Surgery to repair or replace a damaged joint. This is usually not needed until years after diagnosis.
- Ultraviolet light treatment (UVB or PUVA)
Possible Complications of Psoriatic Arthritis:
The condition may damage joints enough to change your activity level. Lack of activity can lead to stiff joints and muscle weakness. Psoriatic arthritis can also cause tiredness (fatigue) and low red blood cell count (anemia). You are more likely to develop:

- Diabetes
- High blood pressure
- High cholesterol
- Obesity
Living with Psoriatic Arthritis:
Exercise keeps your joints and tendons loose and limber and helps you reduce inflammation and pain. Building up your muscles decreases the workload on your joints. Anything that gets your heart pumping and your joints moving will help to lower your risk of developing a comorbid (related) condition.
When you set out on an exercise program, you don’t have to aim for Olympic gold. If you were active before you had PsA, try to maintain a regimen as close to your old normal as possible. If you were inactive, start small. In general, people with PsA can enjoy walking, indoor and outdoor cycling, swimming or warm-water exercise, yoga, and tai chi. A physical therapist or a qualified fitness or health professional can help you create an exercise plan that makes sense for you.


Whichever exercises you choose, your muscles will work extra hard at the beginning. After exercising you might experience soreness. You might have a hard time cooling down. You might even feel worse the next day. This is your body telling you to ease up! Listen to your body to help you learn about the types of activities that tend to induce discomfort or pain.
The opposite can also happen. As soon as any type of activity becomes less than challenging, it’s safe to assume your body has adapted and that it’s time for a new challenge.
Managing Pain:
The inflammation caused by PsA can have short-term effects such as pain and swelling. Inflammation can also cause long-term damage to your joints. Stress is another aggravation. The combination of inflammation and stress can make you even more sensitive to pain.
Talk to your health care provider about the following medications for managing pain, their interactions with other treatments for PsA and their possible short- and long-term side effects.


Nonsteroidal anti-inflammatory drugs (NSAIDs) are over-the-counter medications such as aspirin and ibuprofen as well as prescription drugs. NSAIDs help to decrease inflammation, joint pain, and stiffness. They can also make it easier for you to move.
A health care provider considers stronger medications when NSAIDs and aspirin fall short in their results.
Biologics target specific parts of the immune system (unlike traditional oral systemic drugs, which impact the entire immune system). Although biologics interfere with the process that causes the painful PsA inflammation, you might have to wait at least three months until a biologic begins to reduce your pain. However, recent studies show that biologics very quickly demonstrate a positive effect on your mood.
People with PsA are at greater risk of depression, and depression can heighten your sensitivity to pain.
Other Medications for Pain:
When the pain of PsA is severe or when it does not go away with traditional PsA treatments, you may want to talk to your health care provider about medication that helps reduce your sensitivity to pain.
Prescription pain medications such as Gabapentin and Pregabalin are used to treat neurological pain. Certain anti-depressants called noradrenergic and specific serotonergics (NaSSAs) can reduce your sensitivity to pain as well. Capsaicin, a compound found in chili peppers, has a numbing effect on pain receptors. Applying a local anesthetic like prilocaine can help minimize the initial burning sensation of capsaicin.
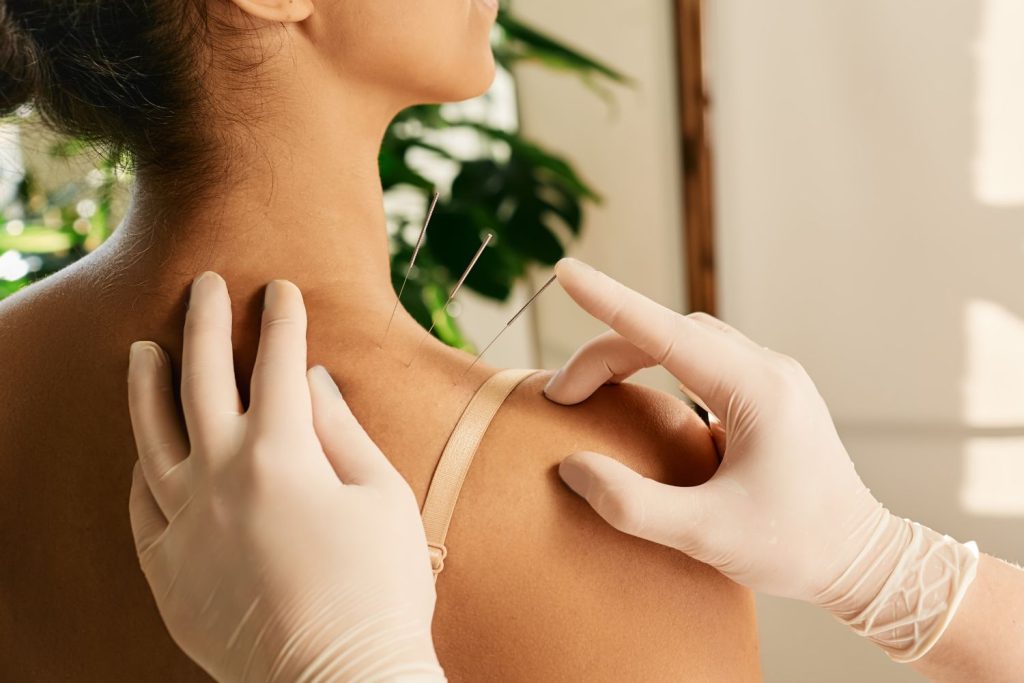

Alternative Treatments for Pain:
Some studies show acupuncture as a valuable option for pain relief. There are no side effects.
Researchers have not studied the impact of meditation on people with PsA, but there is some evidence that practicing what’s called mindfulness meditation can relieve stress.
Show to Hold a Job and Handle PsA:
It’s important to understand your disease, your rights and the resources available to you.
Schedule a meeting with your supervisor at a time when neither of you is under pressure. Describe how your PsA may affect your performance, including scheduling doctor appointments and the use of assistive devices. The goal of this talk is to find the workplace adjustments that will benefit the company, your co-workers and yourself. It’s better to ask for support or adaptations from your employer than to try to push through it on your own and risk a flare-up.

“Assistive devices” covers everything you need to be comfortable and more productive on the job. You might need something as simple as additional breaks or assistance with lifting heavy objects or adjusting the height of your chair and desk and the distance to your computer monitor. You might need equipment, such as switching from a mouse to a track pad or using a writing bird to help you grip a pen. Research options and prices ahead of time. If possible, try new equipment at home.
Your employer may not be required to purchase expensive equipment for you. However, tax deductions and/or tax credits may be available to certain employers who provide accommodations and/or jobs for people with disabilities.
How To Reach Remission?
Some people may have a very mild form of PsA and get it under control relatively quickly, whereas others may have very severe disease and have to try several medications and combinations of medications to find relief. There are no clear criteria for defining remission in PsA, so it is difficult to say when you have gotten there. In general, rheumatologists talk about getting to “a minimal disease activity state
One of the best ways to help achieve low disease activity is through close collaboration with your rheumatologist. After the initial period they will re-evaluate your symptoms, examine your laboratory findings and then adjust the medication as needed. If you’re not responding adequately, your doctor may change or increase the dose of your medication.

Can I Stop My PsA Medication When I Feel Better?
Once you reach a state of low disease activity, rheumatologists recommend you continue on your medications. If you take more than one medication or if your medication comes in different doses, your doctor can try taking you off one medication or lowering the dosage.
Studies show that some patients had a recurrence within six months of stopping medication and most of them flared within the first two to three months. It appears that though the disease may quiet down during remission, it doesn’t cease to exist.
These thoughts likely resonate with other people with cancer and their caregivers, who face similar daily struggles to balance the demands of illness with the need to preserve a sense of normalcy in their lives. Patients who have more consistent, longer duration of disease and patients who have more severe disease are at the highest risk of recurrence. Another risk factor is male gender and evidence of some clinical inflammation on ultrasound.
Can Early Treatment Help Me Achieve Remission?
Starting treatment for psoriatic arthritis as early as possible could, in theory, make lasting remission more likely. Patients with psoriatic arthritis can develop significant damage early in their disease. Unfortunately, many people with psoriasis are unaware they also have PsA, and many patients are undertreated. By treating it early, joint damage can be prevented, leading to improved long-term outcomes.
A patient with PsA for 10 years may have already accumulated some amount of joint damage and possibly deformities limiting the function of their joints. So if you treat them at that point, they may still see significant improvement from treatment, but damage to the joints that has already occurred cannot be reversed.

Although some PsA patients may be frustrated by the need to stay on medication, remission is far better than no remission. One thing to remember is that while these medications work, they don’t cure the disease. However, it is a testament to the effectiveness of current drugs that many patients forget how they felt before, and how affected their joints and skin were prior to being on the medications.
